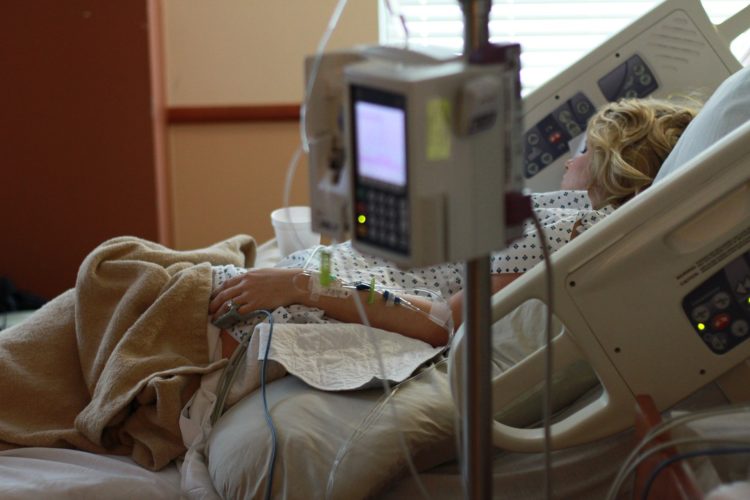
Townsend Article: Melatonin prevents delirium in hospitalized ICU patients.
Kelsey Asplin, ND
Townsend Letter
Issue: December 2019
We’ve been fascinated by the wide range of clinical uses that have been reported for the hormone melatonin. Initially we just thought of melatonin as an agent to improve sleep or help one get over jetlag faster. In the 1990s melatonin’s anticancer effects were added to the list of possible uses. Over the years the list of applications has grown to include reflux disease (GERD), pancreatitis, anxiety and others.
A paper published early in 2019 by Baumgartner et al, has added another possible use for melatonin, one that again catches us by surprise. Melatonin use has been demonstrated to lower risk of delirium in patients hospitalized in intensive care (ICU).
Delirium is a common complication among patients in intensive care units, but treatment options are limited and pose additional risks. It appears that melatonin, a simple and nontoxic intervention, may be an effective therapy for this condition.
By definition patients in ICU are critically ill and ideally any interventions one might choose to reach for to reduce the danger of developing delirium should have little or no added risk for side effects. Melatonin fits this requirement.
As most patients who develop the condition are critically ill, an ideal intervention would be one with a high rate of risk reduction, additional health-supportive actions, and little to no side effects.
Baumgartner’s retrospective, observational cohort study included 232 adults (≥18 years of age): 117 patients in a melatonin group and 115 patients in a control group. Patients were admitted to medical or cardiac ICU between 2013-2017, and those given melatonin were compared to those who did not receive it. Exclusion criteria included use of antipsychotic or sleep medications prior to admission, primary neurologic condition or injury, hepatic encephalopathy, end-stage liver disease, active withdrawal from alcohol use, and any other conditions preventing delirium screening.
Development of delirium was determined by 2 consecutive positive scores on the Confusion Assessment Method for the ICU (CAM-ICU), within a 14-day period after inclusion. Participants in the study were assessed with the CAM-ICU every 12 hours.
The primary outcome measured was whether the patient developed delirium while in the ICU. Doses of melatonin administered were also tracked. A secondary outcome was also tracked, the number of delirium-free days in a 28-day period.
Patients who received melatonin were less likely to develop delirium. The patients taking melatonin had a significantly two-thirds lower rate of delirium compared to the control group (9 [7.7%] vs 28 [24.3%]; P=0.001).
The findings remained consistently significant when assessed in statistical models that controlled for variables that included age, sex, history of hypertension, need for emergent surgery, Acute Physiology and Chronic Health Evaluation II score,s mechanical ventilation, length of stay in ICU, dexmedetomidine use, and benzodiazepine use.
In those who did develop delirium, there was no statistical significance in how long the delirium lasted. Those in the melatonin group experienced 19.9 delirium-free days, compared to 20.9 days in the control group (P=0.72).
Typical starting doses for melatonin were 3-6 mg nightly and doses were titrated up to 9-10 mg as needed for sleep. In the patients who developed delirium, the average dose was 3 mg, with a range of 1-5 mg.[i]
Currently, there are no US Food and Drug Administration (FDA)-approved pharmacological therapies to treat or prevent ICU delirium. Management often relies on antipsychotic medications, which carry their own risk profile, including further neurological impairment and risk of death in older adults with dementia. Obviously older adults are the ones most likely to get delirium in the first place.
Several other, earlier publications have also suggested melatonin might be protective against delirium.
A paper published in March 2019 by Cuismano and colleagues at the Cleveland Clinic looked at factors that might predict which patients were most likely to experience a reduction in delirium risk from melatonin administration.[ii] Martinez and colleagues in Australia announced their intention to run a similar clinical trial to this one back in 2017. [iii] Clayton-Chubb also from Australia had also announced the same intention the year prior.[iv] It seems that Baumgartner’s team beat them to publication. A study done in Iran and published in 2018 failed to prove effectiveness of melatonin against delirium in surgical ICU patients and suggested that the benefit might be more likely seen in those hospitalized for medical reasons.[v] Sarah Joseph’s 2018 article provides an excellent review and summary of this topic and provides a rationale for use. [vi]
While not tracked in the current study, this simple and nontoxic intervention may impact overall outcome. The authors note that “Intensive care unit (ICU) delirium is an acute brain dysfunction that has been associated with increased mortality, prolonged ICU and hospital lengths of stay, and development of post-ICU cognitive impairment.”This implies that further studies using melatonin in this patient population may show even more profound benefits.
Few patients who have endured a night in the hospital will tell you they slept well unless heavily medicated. Melatonin may offer benefit to many hospitalized patients by improving their sleep. This study suggests measurable benefits even in the critically ill.
Melatonin is a natural therapy with many other well-supported uses and generally mild side effects. It’s not entirely clear if melatonin’s usefulness in ICU delirium is grounded in its effects on circadian rhythm regulation (though this is likely one mechanism of action), or some other unknown mechanism. However, as sleep disparity is a concern and a plausible contributing factor in the development of delirium in critically ill patients, this, along with its proposed antioxidant, cardioprotective,[vii] neuroprotective,[viii] hepatoprotective,[ix] and esophago-protective[x] properties (all potentially important actions in the population of chronically ill patients), makes melatonin a viable and encouraging therapy option.
While the study does not provide evidence regarding optimal dose, the data suggest that nightly doses of 3.5 mg or greater may be of more benefit.
But honestly, we can’t think of any vendor that sells 3.5 mg doses of melatonin and so would just suggest using standard 3 mg capsules.
Author bio: Dr Kelsey Asplin is a
naturopathic doctor and an instructor in the Integrative Health Care Program at
Metropolitan State University (MSU) in Denver. She also serves on the board of
the Colorado Association of Naturopathic Doctors. She is a Certified Kinesio Taping
Practitioner™ and graduated from Bastyr University in Seattle, Washington. Dr.
Asplin enjoys working with patients seeking the next level of their wellness
evolution. To learn more about Dr Asplin and her practice, visit her website at
www.drkelseynd.com
[i] Baumgartner L, Lam K, Lai J, et al. Effectiveness of melatonin for the prevention of intensive care unit delirium. Pharmocotherapy. 2019;39(3):280-287.
[ii] Cusimano JM, Welch S, Perez-Protto S, Lam S. Factors Associated With Delirium in Surgical Intensive Care Unit Patients Treated With Supplemental Melatonin: A Case-Cohort Study. Clin Neuropharmacol. 2019 Mar 26.
[iii] Martinez FE, Anstey M, Ford A, et al. Prophylactic Melatonin for Delirium in Intensive Care (Pro-MEDIC): study protocol for a randomised controlled trial. Trials. 2017 Jan 6;18(1):4. doi: 10.1186/s13063-016-1751-0.
[iv] Clayton-Chubb DI, Lange PW. Moderate dose melatonin for the abatement and treatment of delirium in elderly general medical inpatients: study protocol of a placebo controlled, randomised, double blind trial. BMC Geriatr. 2016 Feb 29;16:54.
[v] Abbasi S, Farsaei S, Ghasemi D, Mansourian M. Potential Role of Exogenous Melatonin Supplement in Delirium Prevention in Critically Ill Patients: A Double-Blind Randomized Pilot Study. Iran J Pharm Res. 2018 Fall;17(4):1571-1580.
[vi] Joseph SG. Melatonin supplementation for the prevention of hospital-associated delirium. Ment Health Clin. 2018 Mar 26;7(4):143-146.
[vii] Jiki Z, Lecour S, Nduhirabandi F. Cardiovascular benefits of dietary melatonin: a myth or a reality? Front Physiol. 2018;9:528.
[viii] Shu T, Fan L, Wu T, et al. Melatonin promotes neuroprotection of induced pluripotent stem cells-derived neural stem cells subjected to H 2 O 2 -induced injury in vitro. Eur J Pharmacol. 2018;825:143-150.
[ix] Bonomini F, Borsani E, Favero G, Rodella L, Rezzani R. Dietary melatonin supplementation could be a promising preventing/therapeutic approach for a variety of liver diseases. Nutrients. 2018;10(9):1135.
[x] Majka J, Wierdak M, Brzozowska I, et al. Melatonin in prevention of the sequence from reflux esophagitis to Barrett’s esophagus and esophageal adenocarcinoma: experimental and clinical perspectives. Int J Mol Sci. 2018;19(7):2033.